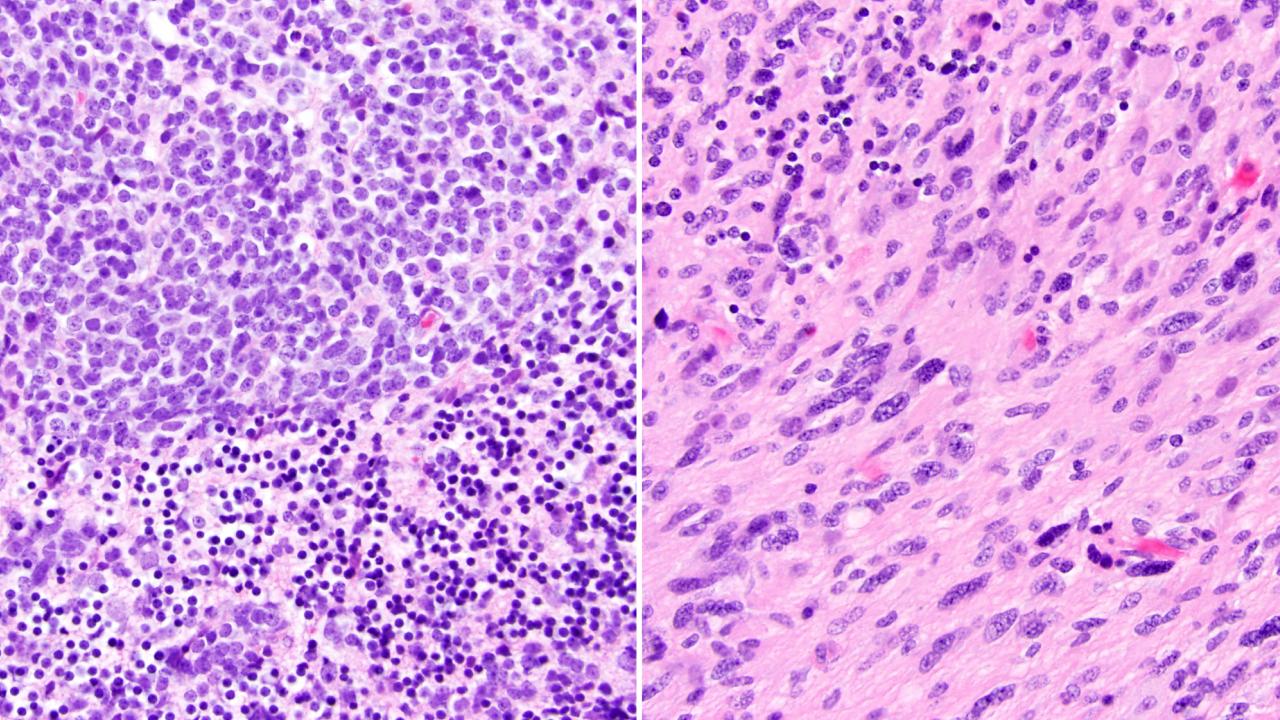
Secondary gliomas can arise following radiation therapy to treat a primary cancer. Pictured here, histology from a patient who was initially treated for medulloblastoma (left) and later developed high-grade glioma (right) following craniospinal radiation.
For many common childhood cancers, radiation therapy can be an effective, even curative, treatment. However, long-term survivors are at risk for developing new, or secondary, cancers as a consequence of radiation, sometimes decades later.
Children with cancers like medulloblastoma and craniopharyngioma are likely to receive intracranial radiation therapy as part of their treatment. A minority of these patients will later develop a secondary brain tumor as a result of radiation; these are often meningiomas or high-grade gliomas.
“Hopefully one day we’ll have more specific targeted medicationsto treat and cure cancer, allowing the avoidance of radiation therapy altogether. But for now, radiation is still a mainstay in the treatment regimen for many cancers,” remarked UCSF neuropathologist David Solomon, MD, PhD.
Secondary cancers represent a major cause of mortality for long-term survivors of childhood cancers, and much remains unknown about how these tumors arise. Recently published in Acta Neuropathologica, Solomon led a team of UCSF clinicians and researchers in the first genomics study of radiation-induced gliomas.
Solomon and his colleagues found that radiation-induced gliomas carry a unique genetic signature that is distinguishable from that of spontaneous gliomas. Radiation, by causing double stranded breaks in DNA, leaves a distinct pattern of chromosomal breakpoints that result from the faulty repair of DNA damage.
They further identified which genes are commonly mutated in radiation-induced gliomas, which are different from those commonly found in spontaneous gliomas.