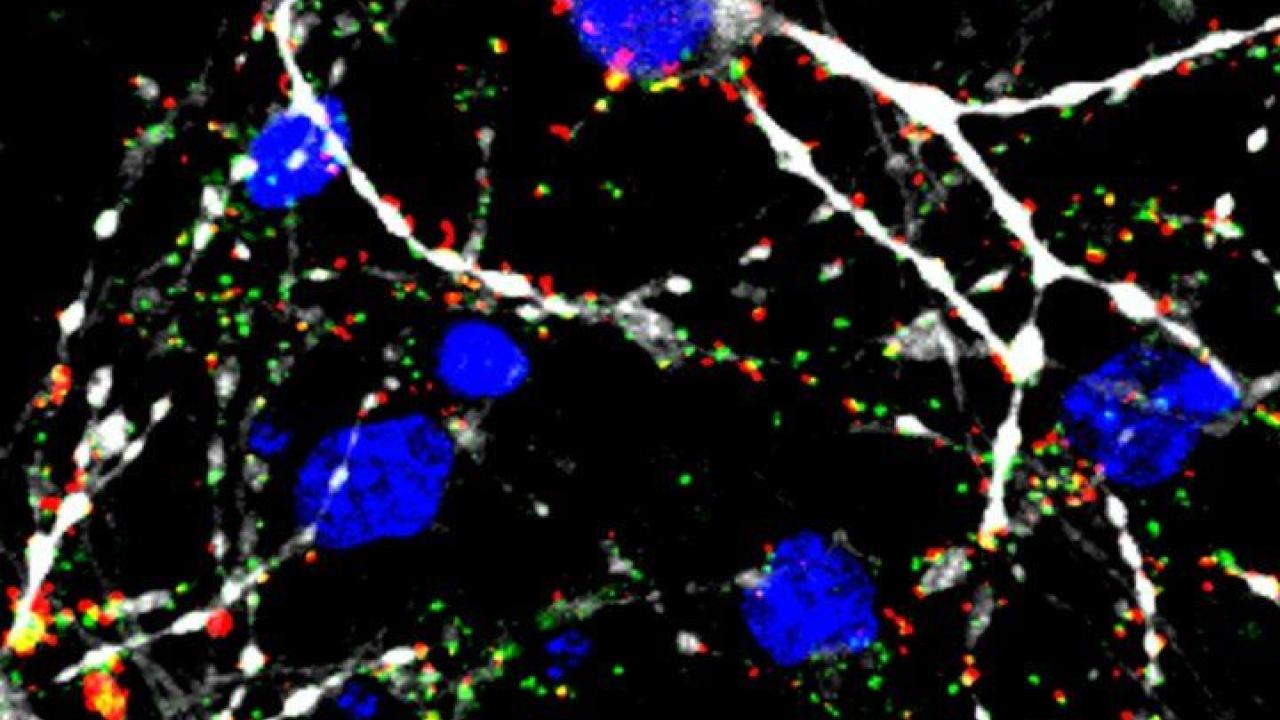
Human glioblastoma cells showing areas where new connections between cells are being formed at an accelerated rate. Image by Hervey-Jumper
The difficult-to-treat brain cancer glioblastoma steals a person’s mental faculties as it spreads, yet the tumor’s insidious ability to infiltrate neighboring networks in the brain could also prove its undoing.
Scientists at UC San Francisco have discovered that neural activity in these deadly tumors can restructure connections in surrounding brain tissue, causing the cognitive decline associated with the disease, and that the drug gabapentin, commonly used to prevent seizures, could block this growth-causing activity in mice with glioblastoma.
The findings, appearing in Nature, provide a hopeful new direction for research on a disease that has defied even the most modern and sophisticated types of cancer drugs.
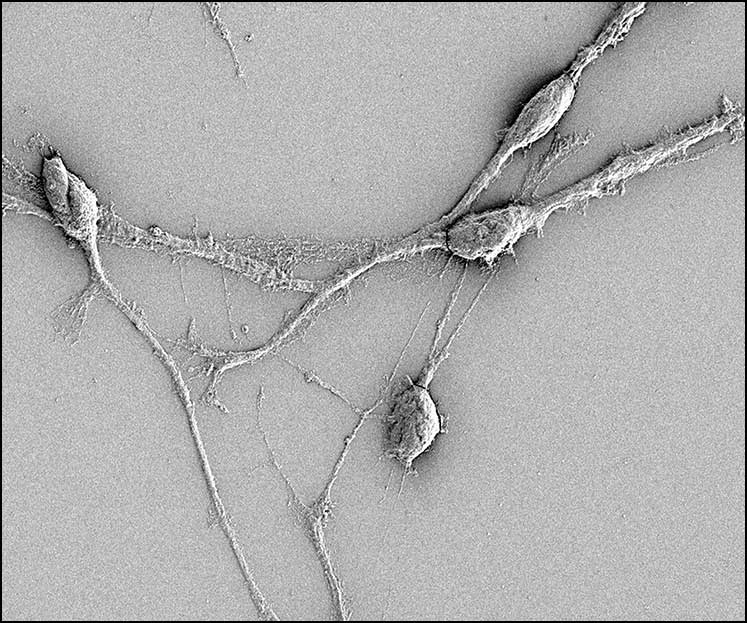
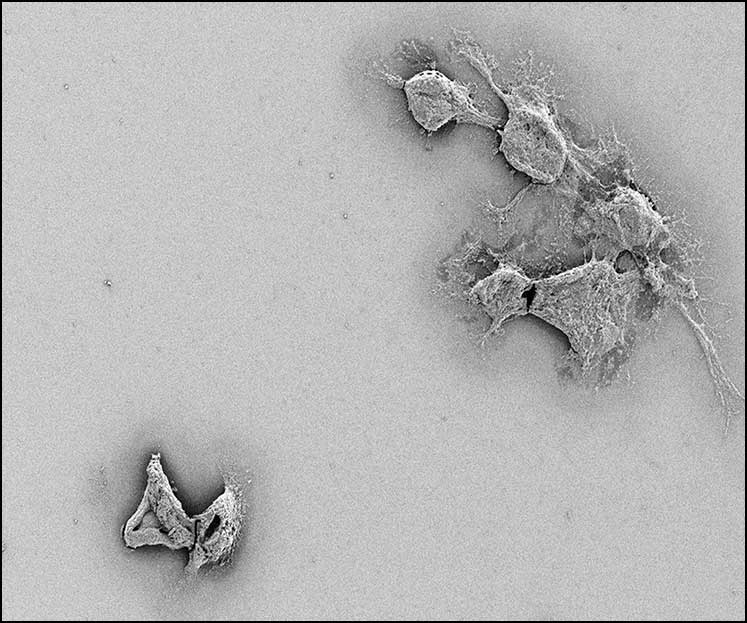
Tumor microtubes, shown above, are continuations of tumor cell membranes extending to other cells.
“Glioblastoma needs a win,” said neurosurgeon Shawn Hervey-Jumper, MD, who led the study along with postdoctoral scholar Saritha Krishna, PhD. “This study opens the door to a whole world of treatment possibilities for these patients and a new way of thinking about brain cancer.”
When Hervey-Jumper was beginning his study, scientists had recently discovered that brain tumors are fueled by a positive-feedback loop. It begins when cancer cells produce substances that can act as neurotransmitters. This “extra” supply of neurotransmitters spurs neurons to become hyperactive, which in turn stimulates the growth of the cancer cells.
Building on earlier studies done on mice and brain organoids (small bundles of neurons derived from human stem cells grown in petri dishes), Hervey-Jumper focused on what the feedback loop meant for human behavior and cognition in brain cancer.
The team recruited volunteers awaiting surgery for glioblastoma whose tumors had infiltrated the brain region controlling speech. Just before operating on the tumor, Hervey-Jumper placed a grid of tiny electrodes on the surface of the speech region, showed the volunteers pictures and asked them to name what they saw.
The research team then compared the results with normal-appearing non-tumor regions of the brain from the same participants. They found that the tumor-infiltrated brain regions used a broader neural network of brain area in the effort to identify what they were seeing.
Cancer as a Conversation Between Cells
Hervey-Jumper attributes this to degradation of information-processing power in that region of the brain. He likens it to an orchestra where it’s the musicians playing in synchrony that makes the music work.